11 MOST OVERLOOKED ESOPHAGUS CANCER SYMPTOMS
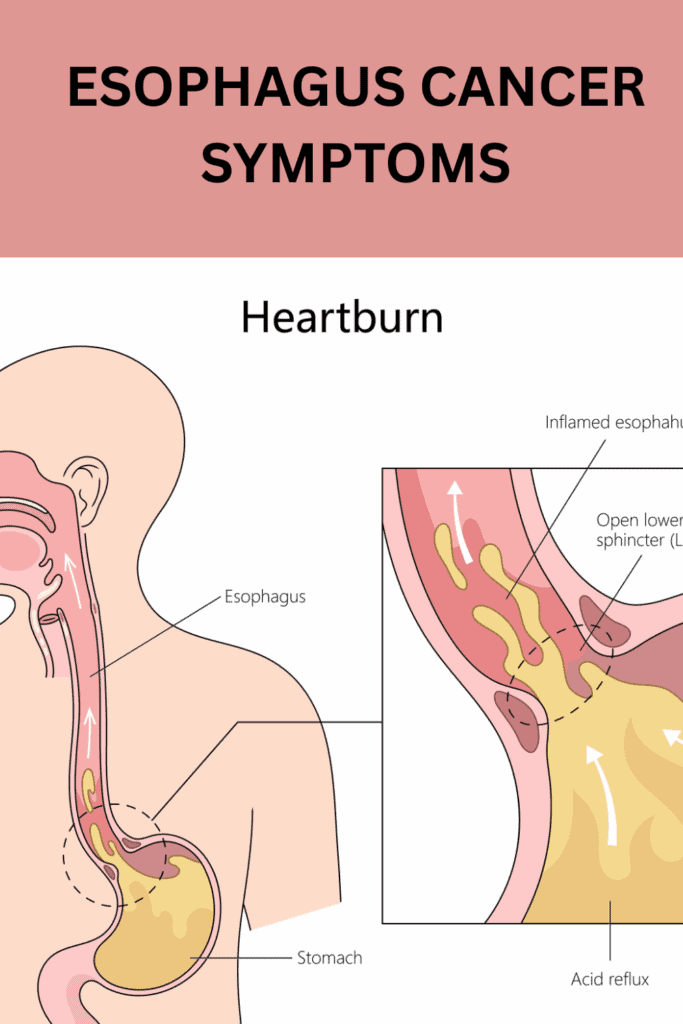
ESOPHAGUS CANCER SYMPTOMS CAN BE TRICKY
Esophagus cancer symptoms can be sneaky—especially when you’ve lived for years with reflux and constipation and chalk everything up to “that’s just my stomach.” If that sounds like you, lean in. I’m writing this in second person so it speaks directly to your gut (pun intended), but I’ll weave in my own journey as a wake-up call: I finally went in for a long-overdue colonoscopy after 10 years without one, my GI doctor added an endoscopy “just to be safe,” and—boom—tests revealed stage 3 esophagus cancer and stage 1 colon cancer. My life changed in July 2023. Your life might change today if you take the next step.
WHY YOU MIGHT OVERLOOK ESOPHAGUS CANCER SYMPTOMS (“when reflux and constipation are your “normal”)
When you’ve battled reflux since college, when constipation shows up like an uninvited roommate, and when nausea shadows your days, you get used to pushing through. You switch to liquids because food sounds awful. You sleep with a pillow pressed to your chest and a heating pad on your belly. You tell yourself, “I’ll feel better tomorrow.” That’s exactly how esophagus cancer symptoms hide—in plain sight—inside habits you’ve learned to normalize.
I had bouts of nausea so intense I skipped meals, felt pale from low nutrients and low hydration, and sometimes noticed small amounts of blood in my stool. I even had nights after heavy drinking (I’ve now been sober 9 years) when I vomited and saw streaks of blood. I’d bloat so much from constipation I looked seven months pregnant. I remember crying on the bathroom floor, straining so hard the veins stood out in my neck. If any of this is familiar, please keep reading and please, please talk with your doctor.
Spotlight: THE BIG “3” ESOPHAGUS SYMPTOMS SIGNALS TO TAKE SERIOUSLY
These three patterns show up again and again in stories like mine. If they’re your “normal,” don’t ignore them—tell your doctor.
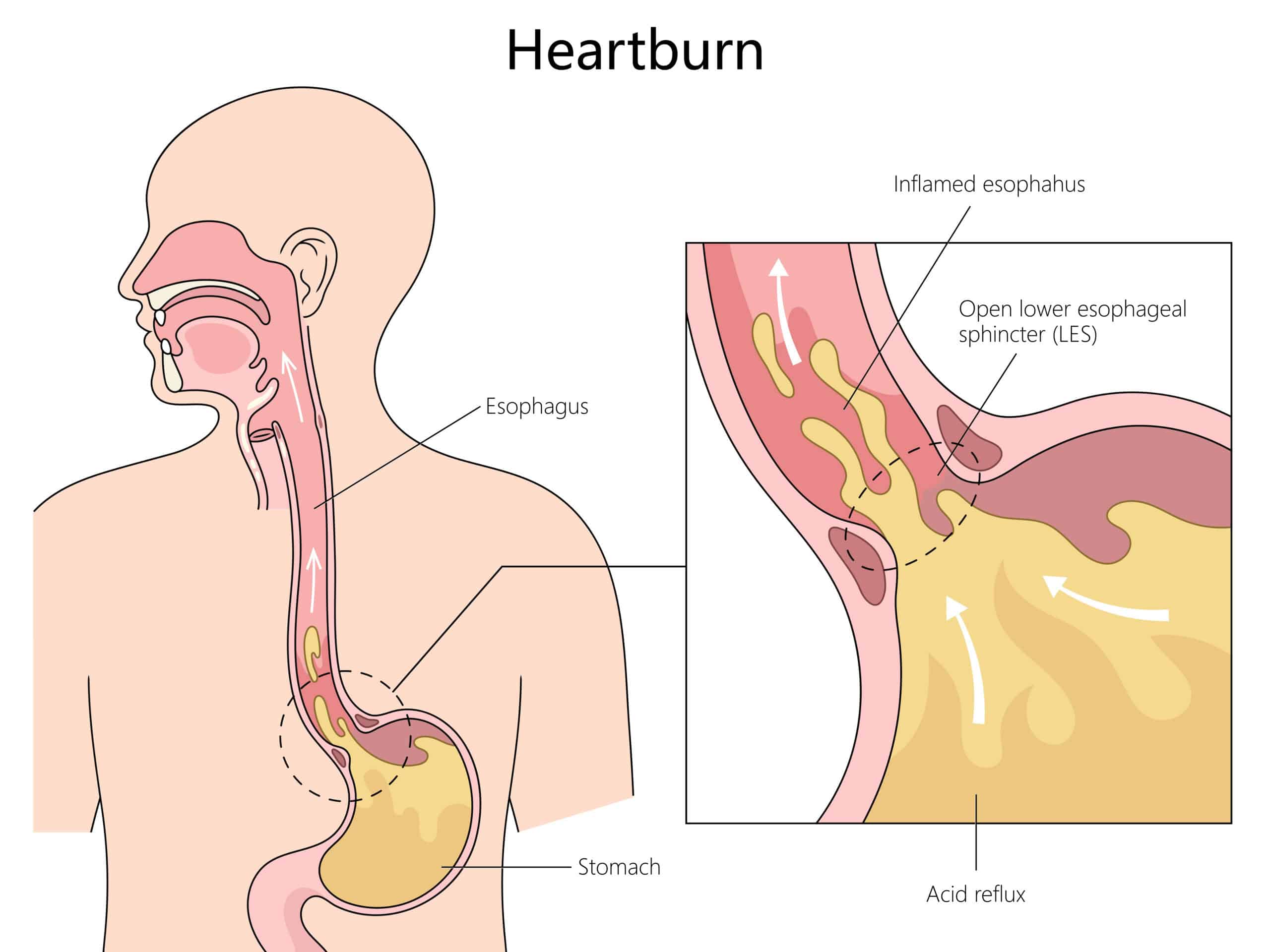
1) Reflux that changes or worsens
- Heartburn climbs higher in your throat, wakes you at night, or stops responding to meds.
- New burning, bitter taste, or more throat clearing/hoarseness.
- Paired with trouble swallowing or chest pressure? Double-flag.
2) Constipation that’s severe or escalating
- Balloon-level bloat, heating-pad nights, or straining until veins pop.
- Long gaps between bowel movements, then small amounts of blood in stool.
- Constipation + nausea + fatigue can hide nutrition decline.
3) Alcohol history with irritation/bleeding
- Past heavy drinking (or current use) plus vomiting episodes, blood streaks, or worsening reflux.
- If alcohol’s in your story (mine too), be proactive: ask about endoscopy even if you think you’re “too young.”
Keep these “Big 3” in mind as you read the full symptom list below. They’re your quick gut-check for esophagus cancer symptoms.
OFTEN-OVERLOOKED ESOPHAGUS CANCER SYMPTOMS
1) Trouble swallowing (dysphagia)—solids first, then sometimes liquids.
You cut food smaller, switch to soups/shakes, or feel bites “stick.” That’s a hallmark esophagus cancer symptom.
2) Persistent heartburn or worsening reflux.
If reflux meds stop working or the burn creeps higher, tell your doctor.
3) Chest discomfort, pressure, or back pain unrelated to exercise.
Sternum pressure or mid-back ache you keep blaming on reflux is a red flag if it’s new or escalating.
4) Unexplained nausea and early fullness.
Feeling “done” after a few bites isn’t just picky eating. It’s common with esophagus cancer symptoms, constipation, and reflux.
5) Unintentional weight loss or nutrition decline.
Hard swallowing + nausea → fewer calories and nutrients. You can look washed out and weak.
6) Hoarseness, chronic cough, or throat clearing.
Acid irritation plus swallowing changes can overlap with esophagus cancer symptoms.
7) Bleeding signs: blood in stool or spit/vomit.
Even small amounts of blood in stool need evaluation. Streaks with vomiting/spit—get checked. Colonoscopy + endoscopy matter.
8) Fatigue that doesn’t match your schedule.
Low iron from slow blood loss or poor intake can wipe you out.
9) Bloating and severe constipation that escalate.
“Seven-months-pregnant” bloat, nightly heating-pad dates, or straining to tears? Not normal—get help.
10) A “something’s off” feeling you can’t shake.
You know your body. If reflux is different, constipation is worse, and energy is sliding—listen to that nudge.
11) Frequent regurgitation—food or sour fluid coming back up after swallowing.
Not just heartburn—actual backflow shortly after meals (especially with lying down) is another overlooked esophagus cancer symptom and pairs often with reflux
THE DAY YOU DECIDE TO GET ANSWERS (My Story As Your Nudge)
Here’s the fork in the road: I finally got my health insurance back. I hadn’t had a colonoscopy in 10 years. My GI said, “Let’s add an endoscopy for safety.” That extra step saved my life. The scope showed esophagus cancer (stage 3) and colon cancer (stage 1). The esophagus cancer was the bigger immediate fight. That was July 2023, and it set me on a journey of treatment, faith, grit, and lifelong adjustments—physically and mentally.
At the very start, I had just begun a relationship with a wonderful veterinarian. By God’s grace and guidance, he became my backbone. He and my brother were my lifeline. That support, plus sober years behind me, gave me strength to face what came next. If you’re reading this and recognizing your own symptoms, I want you to have your lifeline and your next step—today.
WHAT TO DO IF YOU SEE YOURSELF IN THESE ESOPHAGUS CANCER SYMPTOMS
A) Call your doctor now and report specifics.
Say: “I have difficulty swallowing solids,” “I’ve had small amounts of blood in my stool,” “Nausea keeps me from eating,” “I bloat severely from constipation,” “Food comes back up after I swallow,” “I’ve lost weight without trying.”
B) Ask whether you need an upper endoscopy in addition to a colonoscopy.
If you’re due (or overdue) for colonoscopy, schedule it. With long-standing reflux, swallowing changes, regurgitation, or bleeding, ask about endoscopy. One found my colon issue; the other found my esophagus issue.
C) Track a 2-week symptom log.
Record meals, any “food sticking,” nausea, reflux flares, regurgitation, bowel movements, any blood (color/amount), energy, hydration, and sleep. SEE DIGESTIVE ARTICLE BELOW:
D) Know when to seek urgent care.
Go now if you have black/tarry stools, vomit blood, can’t swallow even liquids, feel faint, or have sudden severe chest pain.
RISK PATTERNS WORTH MENTIONING OUT LOUD
- Long history of reflux (GERD).
- Tobacco or heavy alcohol use, past or present (I’m nine years sober now).
- Male sex, older age, or obesity.
- Diet and lifestyle: poor nutrition, dehydration, and low sleep; constipation often rides shotgun.
None of these automatically mean you have cancer. They’re reasons to stop normalizing pain and start investigating esophagus cancer symptoms—especially if reflux and constipation are longtime companions.
PatchAid Vitamin Patch Corner (how I get my vitamins when swallowing is hard)
Swallowing pills can be tough—especially with esophagus cancer symptoms, reflux, and constipation. I use PatchAid vitamin patches to support my vitamin intake when pills feel like a chore.
- Why I like them: no swallowing, simple routine, easy on busy days.
- My routine: clean, dry skin at night → apply patch → remove the next day → repeat as directed.
- Important: this is my personal routine; always ask your own doctor which vitamins you need and whether patches are right for you.. PatchAid www.patchaid.com/TEXASKK AND PUT IN DISCOUNT CODE TEXASKK FOR 40% OFF
HOW FAITH, SUPPORT AND ACTIONS FIT TOGETHER
I believe God met me at the exact moment I said, “I can’t ignore this anymore.” He provided a partner who stood shoulder-to-shoulder with me, and a brother who never once let go. You deserve that kind of circle—and you deserve an answer about what’s going on in your body. Your action today—calling your doctor, scheduling colonoscopy and asking about endoscopy—is a prayer in motion.
If you have a history of alcohol abuse, I’m speaking straight to you: even if you feel “too young,” even if your pride says “I’m fine,” get the exams. I’ve had nights with a pillow clutched to my chest and a heating pad on my belly because reflux and constipation were running my life. I’ve had the tears, the straining, the bloat, the nausea, the paleness. I’m telling you in love: your body is talking. Listen.
YOUR SIMPLE NEXT-STEPS CHECKLIST
- Call your primary care or GI today. Use the words: “I have several esophagus cancer symptoms alongside long-standing reflux and constipation. I need to be evaluated.”
- Book the tests you’re due for. Overdue for colonoscopy? Schedule it. With your symptom mix, ask if an upper endoscopy should be added.
- Start a 14-day symptom & nutrition log. Track swallowing, pain, reflux flares, regurgitation, constipation, any blood, weight changes, hydration, and sleep.
- Recruit two supporters. A ride-along + an accountability buddy.
- Dial in basics while you wait. Small, frequent meals; soft foods; hydrate; prioritize sleep.
- If you drink, pause now. Even a short break can reduce irritation while you’re getting answers.
- Pray, breathe, and refuse panic. Courage = fear + action. You’re already doing it.
A WORD ON “YEARLY ” SCOPES
People ask if everyone should get annual colonoscopy and endoscopy. Screening schedules are individualized. Many healthy adults don’t need annual colonoscopy; some need them more often due to findings or family history. What you can do today: tell your clinician about your reflux, constipation, regurgitation, bleeding, swallowing difficulty, and any past alcohol/tobacco use. Then ask, “What schedule is right for me?” If your symptoms are active now, evaluation shouldn’t wait.
CLOSING ENCOURAGEMENT
I didn’t plan to discover esophagus cancer the day I finally handled my health checklist. But I’m grateful I did. July 2023 started a chapter I never wanted, and yet it became the doorway to healing, faith, and the kind of love that shows up when life gets hard. If you’ve been living with reflux and constipation, brushing off nausea, ignoring small amounts of blood in stool, noticing regurgitation, or sipping liquids because solids feel scary—this is your sign. Don’t wait for a “perfect time.” There isn’t one.
There is a phone call you can make today. There is an appointment you can put on the calendar. There is a test that can give you answers. And there is a God who sees you taking that brave first step.For anyone skimming for the exact phrase one more time: esophagus cancer symptoms matter. Reflux matters. Constipation matters. Your story matters. Take action—and let your support system (and your future self) thank you for it
Proudly powered by WordPress