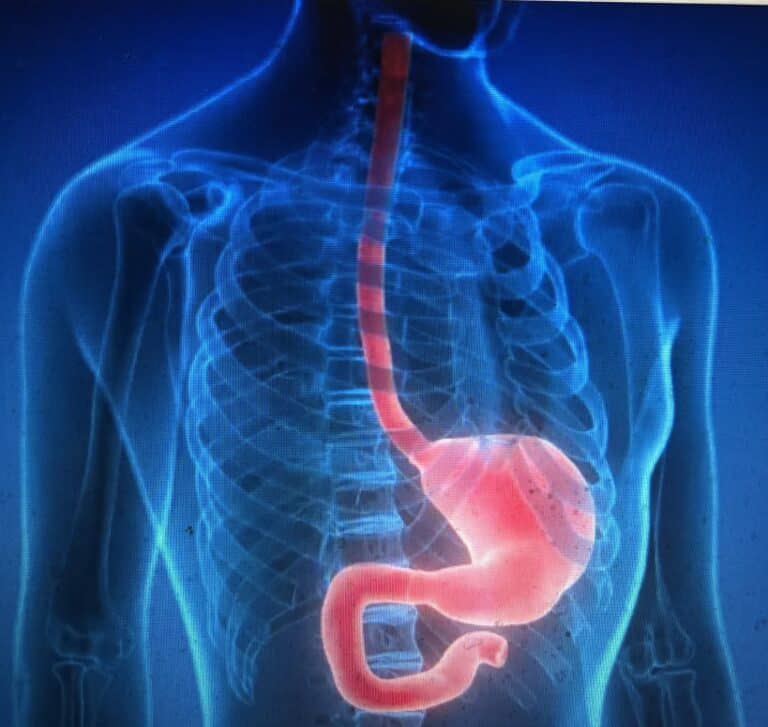
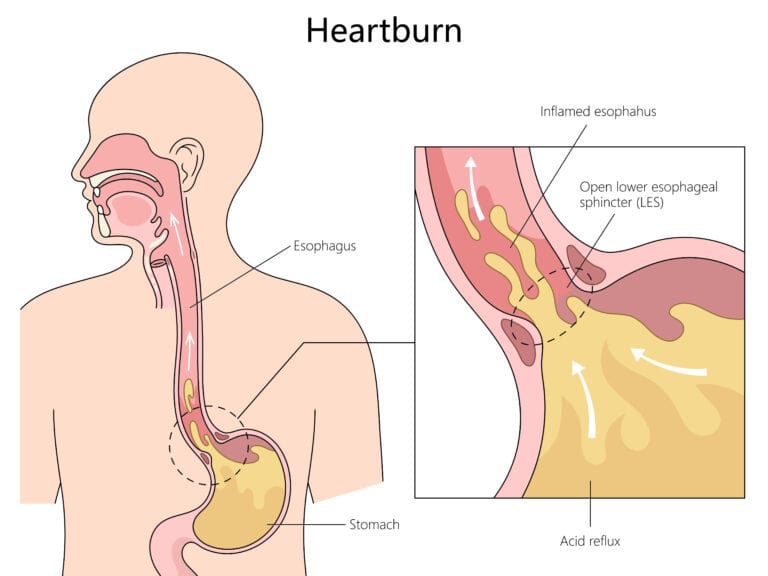
5 ESSENTIAL STAGES OF ESOPHAGUS CANCER GRIEF
If you’re here, you or someone you love is probably wrestling with esophagus cancer grief—that tangled knot of feelings that shows up before, during, and (surprisingly) after treatment. Quick truth from both my heart and what cancer orgs say: the five stages—denial, anger, bargaining, depression, acceptance—are not a straight line. They can overlap, repeat, or show up sideways. And that’s okay.
Here’s my twist: my deepest grief during esophagus cancer didn’t hit during chemo, radiation, or surgery. I didn’t have time for it. I stayed positive by staying (honestly) a little ignorant. I followed directions, trusted my doctors and my God, and put one foot in front of the other. The heavy Esophagus Cancer grief rolled in after surgery—when the monitors were quiet and reality got loud. That’s when I realized: life was beautiful, but it would never be exactly the same. This article weaves the classic five stages of Esophagus Cancer Grief with my own lived journey so you feel seen, equipped, and never alone.

Stage 1: Denial (aka “Just do the next thing”)
What it is (plain talk): Shock, disbelief, and a brain that goes, “Nope—not me.” Denial can look like numbness or hyper-focus on tasks instead of feelings.
How it looked for me:
During diagnosis and treatment, I didn’t want to know everything. I asked for the need-to-know, nothing more. I kept my head down, trusted my care team, and leaned on God. That “ignorance” wasn’t weakness—it was a survival strategy. I didn’t have bandwidth for statistics or worst-case spirals; I had energy for obeying instructions, praying, and showing up.
Helpful moves:
- Short checklists over long research rabbit holes
- A tiny circle of people who can carry details for you
- Prayer over panic; sleep over scrolling
- Permission to say, “Not today. Just tell me the next step.”
Esophagus cancer grief note: Denial protects you until you’re ready. Let it.
Stage 2: Anger (and where to aim it)

What it is: Heat after the numbness. Anger at the disease, the timing, your body, the system, even at God—or at nothing specific at all.
How it showed up for me:
When the fog lifted, I found flash-frustrations—at food that no longer loved me back, A voice that was weaker and hard to understand , a fatigue that stole plans, at the mirror, at well-meaning comments. I also felt mad at how little control I’d had. I told God the honest truth about it (spoiler: He already knew) and He held me anyway.
Helpful moves:
- Name it without shame: “I’m angry because ______.”
- Move it through your body: a walk, a cry, a journal page, a song in the kitchen
- Set gentle boundaries with people and with your own self-talk
- Aim anger toward advocacy: a smart question for your doctor, a small change you can make today
Esophagus cancer grief note: Anger is not a moral failure. It’s your nervous system asking for care.

Stage 3: Bargaining (the “If/Then” trap)
What it is: Trying to negotiate with life—“If I do X, then Y won’t happen.” Sometimes it’s “God, I promise I’ll ___ if You’ll just ___.”
How it surfaced for me:
I noticed sneaky deals in my head: “Once the scans are clear, I’ll never complain.” Or “If I follow the perfect plan, I’ll feel exactly like before.” My breakthrough came when I realized God wasn’t asking for a contract; He was offering companionship. My doctors weren’t giving me guarantees; they were giving me guidance.
Helpful moves:
- Swap deals for direction: “What’s the next wise step?”
- Track what helps (foods, timing, movement, meds)—no perfection needed
- Ask your care team, “What would you prioritize if you were me?”
- Keep promises small and doable: drink water, take a short walk, keep a gratitude line
Esophagus cancer grief note: Bargaining isn’t bad; it’s fear looking for a handle. Replace deals with daily practices.

Stage 4: Depression (sadness that deserves a seat)
What it is: A deep dip when the reality lands—loss of energy, tears, withdrawal, “What now?” This is common and human.
How it met me:
After surgery, when the calendar got quieter, the losses spoke louder: foods I miss, social ease I once had, the difficulty of talking and being heard or understood ,the old autopilot. I cried. I slowed down. I told my family what I needed. I also talked to God—and sometimes one of my preachers at Prestonwood Baptist Church—about heavy days. Feeling grief didn’t cancel my gratitude. Both can live in the same heart.
Helpful moves (and a gentle safety note):
- If sadness lingers or feels heavy, tell your doctor; help exists
- Create a “low day” routine: soft foods, soft clothes, soft music, short walk, early bed
- Journal prayers: “Here’s what hurts. Here’s what helped today. Thank You for ___.”
- Invite one person into your real story this week
Esophagus cancer grief note: Depression is a signal, not a sentence. It often needs time, support, and sometimes clinical care. You’re not failing—you’re healing. An Excellent informative site and tons of information on support groups is https://www.texasoncology.com/patients/resources/support-groups
Stage 5: Acceptance (not giving up—growing up)
What it is: A clearer, calmer relationship with your reality. Not fake-smiling. Not surrendering hope. A grounded yes to what is, so you can work with it.
How I live it now:
I’m more present. I move slower and love deeper. My voice is different that has caused some insecurities but made me more compassionate and I notice what my body likes and dislikes and respect those boundaries. I want to be more like God—patient, kind, others-centered. I feel more driven to help, to pray, to share honestly. Acceptance, for me, is staying active and present: I keep learning, keep adjusting, keep praising.
Helpful moves:
- Build “new normal” routines: meal timing, movement windows, rest rituals
- Serve someone else—purpose lifts pain
- Celebrate small wins: better sleep, less reflux, a good walk, a kind word
- Keep gratitude simple and daily
Esophagus cancer grief note: Acceptance doesn’t end grief; it redeems it. You and your life can be different and deeply good.
Not Linear. Not Prescriptive. Still Helpful.
Cancer orgs say it and I co-sign it: you won’t necessarily march through these stages in order. You might skip one, repeat another, or feel two at once. That doesn’t mean you’re doing grief “wrong.” It means you’re human. Your esophagus cancer grief is your own—it deserves patience, not rules.
My Before → Bridge → After (the transformation in real life)
Before:
Fast pace, less awareness, “power through” vibes. I tried to outrun discomfort and kept a lot to myself.
Bridge:
Diagnosis, treatment, surgery—and then the five-stage swirl: denial kept me moving, anger found its voice, bargaining tried to make deals, depression asked for gentleness, acceptance taught me presence. Through it all: I trusted my care team and clung to God.
After (in progress):
- Presence over pace. I’m here for the moment I’m in.
- Clarity. I listen to my body—what it loves and what it leaves.
- Relationships. Gratitude deepened my bonds with family and friends.
- Holy resilience. Fear got quieter; faith got sturdier.
- Purpose. I’m more driven to help others beat back fear, find hope, and feel held.
These are the results of walking through esophagus cancer grief with intention: a steadier spirit, a kinder inner voice, and a life that’s measured by faithfulness, not speed.
A Gentle Plan You Can Start Today
- Name your now. “Today feels like anger,” or “I’m in aftershock.” Naming reduces shame.
- One tiny victory. Ten-minute walk, a soothing meal, or a phone-free hour.
- Ask one wise question. To your doctor: “Given my situation, what’s the next best step?”
- Truth + prayer. Tell God what you actually feel. Ask for what you need.
- Community touch. Post a request on the Prayer Wall or text a trusted friend
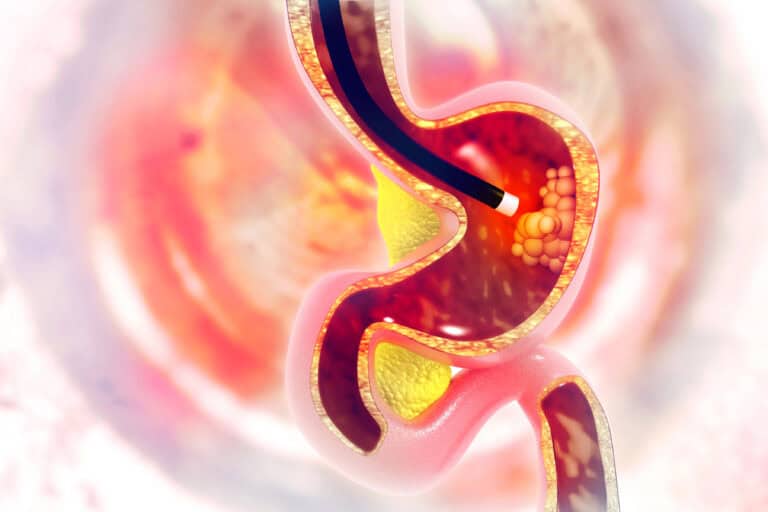
- After my esophageal surgery—where part of my esophagus was removed and my stomach was reconnected higher up—swallowing vitamins, medications, or anything bigger than a seed just wasn’t possible. PatchAid www.patchaid.com/TEXASKK AND PUT IN DISCOUNT CODE TEXASKK FOR 40% OFF. Vitamin patches became my simple workaround: I place one on clean, hair-free skin (for me, that’s my abdomen) at night, since their FAQ says you can wear them day or night, typically for about 8 hours, and rotate spots as needed. They’re designed for transdermal use and made with hypoallergenic, latex-free materials—so it’s no pills, no fuss, just stick and go. My lab work has backed up how well this routine is working for me, and it lets me focus on healing without choking down capsules. As with any supplement, remember PatchAid states their products haven’t been evaluated by the FDA and aren’t intended to diagnose, treat, cure, or prevent disease—so check with your care team first. DURING ALL THE STRESS, I RELIED ON PATCHAIDE PATCHES TO KEEP MY BODY BALANCED. THE 4 I ALWAYS USE IS MULTIVITAMIN,D3,NAD,B12 AND ADD ONE DIFFERENT ONE EACH QUARTER.
For Caregivers & Friends (how to love us well)
- Ask, “Would you like solutions or just company?”
- Offer specific help: school pickup Tuesday, soft-meal drop-off, quiet fold-laundry hour
- Celebrate ordinary wins with us
- Pray with us—even a one-sentence prayer matters PRAYER WALL WWW.TEXASKKSTOMPSCANCER.COM
Faith Note (what steadies me)
I was a Volunteer Hospice Coordinator for 5 years while working real estate in East Texas. I watched love ones and staff grieve for someone that died and all the different ways they grieved. I learned to LISTEN and be in the moment with each person. I prayed for them and I told God my fear and my anger; He gave me peace that didn’t make sense on paper. I thanked Him for a care team that knew what to do when I didn’t. I thanked Him for my family, who held me when I finally had time to cry. If you’re in any stage of esophagus cancer grief, I’m praying this for you:“Lord, meet my friend right where they are. Give courage for today, rest for tonight, and hope for tomorrow. Use this story for good.” Amen.