7️⃣ POWERFUL TRUTHS ABOUT DUODENUM SPASM YOU NEED TO UNDERSTAND
INTRODUCTION: WHEN DIGESTION NO LONGER FEELS SAFE
You know your body in a way most people never have to learn.
After walking through esophageal cancer, colon cancer, radiation, chemotherapy, surgery, and recovery, you became tuned in to every internal signal. So when eating no longer felt nourishing—but instead felt tight, painful, and unpredictable—you knew something deeper was happening.
Duodenum spasm doesn’t always appear clearly on scans. It doesn’t always fit neatly into a diagnosis box. Yet when it shows up, it can quietly take over your life—turning meals into moments of hesitation, discomfort, and fear.
You noticed pressure instead of relief after eating. Cramping that came without warning. A deep internal tightening that forced you to stop mid-meal, sit upright, breathe deeply, and wait for your body to release.
This article exists because what you experienced is real—and because many people live with this silently, unsure how to explain it or where to find answers.
WHAT IS A DUODENUM SPASM?
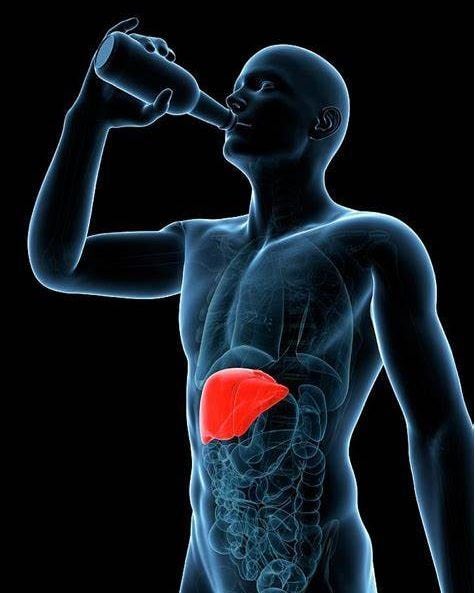
The duodenum is the first portion of the small intestine. It sits just beyond the stomach and plays a critical role in digestion. This is where stomach contents mix with bile and pancreatic enzymes so nutrients can be absorbed properly.
A duodenum spasm occurs when the muscular walls of this section contract too forcefully, too long, or out of coordination. Instead of smooth movement, digestion stalls. Pressure builds. Pain follows.
The duodenum is controlled by:
- The enteric nervous system (often called the “second brain”)
- The vagus nerve
- Digestive hormones that respond to food type and volume
When these systems fall out of sync—often after trauma, surgery, radiation, or prolonged inflammation—the duodenum can tighten defensively rather than flow naturally.
This is not imagined pain. It is altered physiology.
WHY DUODENUM SPASM IS COMMON AFTER CANCER TREATMENT
Cancer treatment saves lives, but it changes the body permanently.
Medical research shows that post-treatment digestive complications increase after:
- Upper gastrointestinal surgery
- Radiation to the chest or abdomen
- Chemotherapy that affects nerve tissue
- Chronic inflammation
Your digestive system endured trauma in order to save you. Scar tissue formed. Nerves adapted. Acid exposure changed. Hormonal signaling shifted.
When digestion began to feel foreign, it wasn’t because your body failed—it was because it survived.
This is why post cancer digestive complications often show up months or even years after remission. The body remembers.
HOW DUODENUM SPASM FEELS IN REAL LIFE
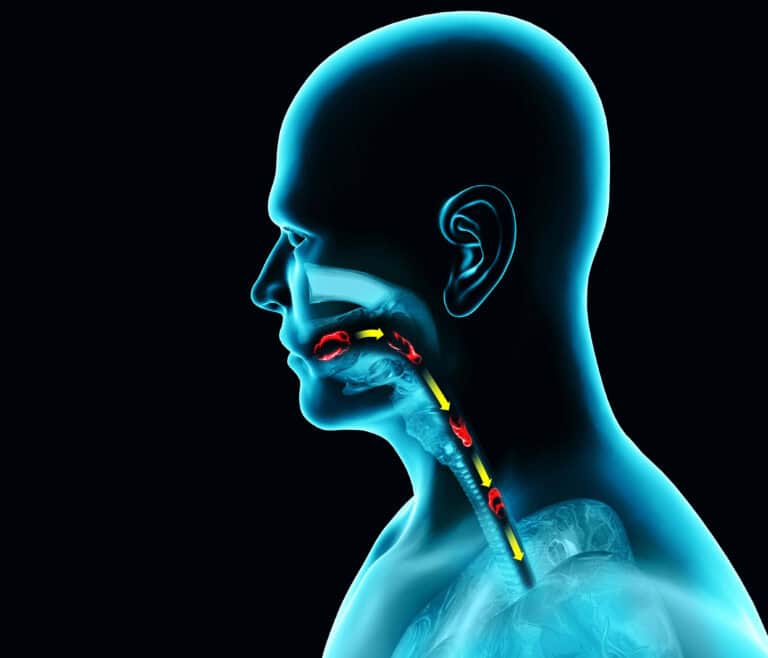
Unlike acid reflux, symptoms often begin after food moves into the intestine.
Common experiences include:
- Upper abdominal cramping after eating
- Deep internal pressure
- Bloating that does not release
- Nausea without vomiting
- Tightness that radiates into the chest or back
You’ve lived the moment where you had to stop eating, sit still, and wait it out. That waiting—hoping your body would soften—can feel endless.
Doctors may label this as a functional gastrointestinal disorder, meaning symptoms are real even when imaging looks “normal.” Functional does not mean insignificant. It means the problem lies in movement and signaling, not structure.
THE NERVOUS SYSTEM CONNECTION YOU CAN’T IGNORE
Your gut and your brain are in constant conversation.
After cancer, the nervous system often remains in a heightened state of alert. The vagus nerve—which plays a major role in digestion—may lose flexibility. Instead of relaxing during meals, the gut braces.
Research on vagus nerve digestion confirms that stress, trauma, and fear directly affect intestinal motility. When the body senses threat, digestion tightens.
You noticed symptoms worsened during emotional days, busy schedules, or rushed meals. That awareness matters. It means your body is communicating—not malfunctioning.
WHY DUODENUM SPASM IS OFTEN MISDIAGNOSED
This condition frequently mimics:
- GERD
- Gallbladder pain
- IBS
- Anxiety
But there are differences:
- Pain builds gradually
- Relief takes time
- Pressure feels gripping rather than burning
- Warmth and breathing help
You knew your pain wasn’t “in your head.” You lived it in your body.
SCAR TISSUE, RADIATION, AND GUT MOVEMENT
Even microscopic scar tissue affects how the intestine moves.
Studies show that intestinal spasms after surgery and digestive spasms after radiation occur because tissue loses elasticity and nerve signaling becomes distorted.
Instead of accommodating food, the duodenum tightens defensively.
That explains why:
- Smaller meals felt safer
- Gentler textures mattered
- Forcing “normal eating” made things worse
Your body wasn’t rejecting food. It was protecting itself.
HOW DIGESTIVE HORMONES CONTRIBUTE TO SPASM
Digestion is guided by hormones as much as muscles.
The duodenum responds strongly to:
- Cholecystokinin (released with fat intake)
- Secretin (released when acid enters the intestine)
- Gastrin (regulates acid and motility)
After cancer treatment, hormone signaling can become exaggerated or mistimed. This explains why high-fat meals often triggered symptoms and why simpler foods felt calmer.
WHY PORTION SIZE MATTERS MORE THAN CALORIES
For a sensitive duodenum, volume matters.
Motility research shows that overstretching the intestine increases spasm risk, especially when nerve sensitivity is high. Smaller portions allow digestion to proceed without triggering defense.
You learned:
- Smaller meals = less pressure
- Slower eating = fewer symptoms
- Stopping early = more comfort
That wasn’t restriction. That was regulation.
THE ROLE OF POSTURE AND TIMING
Posture directly affects digestion.
Sitting upright:
- Improves gastric emptying
- Reduces intestinal pressure
- Supports coordinated movement
Lying down too soon removes gravity and increases discomfort. Remaining upright for 30–60 minutes after meals helps prevent spasm.
You adjusted naturally—another example of listening wisely.
BREATHING AS A TOOL FOR RELIEF
Deep diaphragmatic breathing activates the vagus nerve and shifts the body out of fight-or-flight.
When symptoms hit, you learned to pause, breathe slowly, and wait rather than panic. Research supports this approach. Breathing tells the gut it is safe.
Your breath became medicine.
FOODS THAT TRIGGER DUODENUM SPASM
Common triggers include:
- Fried or fatty foods
- Acidic sauces
- Carbonated drinks
- Large meals
- Eating too quickly
You didn’t just change what you ate—you changed how you ate. That shift mattered.
FOODS THAT HELP CALM THE DUODENUM
Clinical nutrition guidance supports:
- Smoothies and blended foods
- Warm soups and broths
- Soft vegetables
- Lean proteins
- Oatmeal and rice
You once said you never imagined drinking fruit-and-vegetable smoothies every morning. Now they’re part of your healing rhythm—along with daily vitamins, walking two miles most days, and playing competitive tennis twice a week.
That is not surrender. That is strength.
MOVEMENT AS MEDICINE
Moderate, consistent movement improves gut motility and nervous system regulation.
Your walks and tennis:
- Improve circulation
- Enhance vagal tone
- Reduce spasm frequency
Movement reassures the body.
THE EMOTIONAL WEIGHT OF DIGESTIVE PAIN
Digestive pain affects confidence, social life, and joy.
You’ve felt:
- Anxiety around meals
- Fear of eating in public
- Frustration with unpredictability
Medical literature confirms that chronic digestion pain after cancer carries emotional weight. Giving yourself permission to adapt is not weakness—it’s wisdom.
PATCHAID VITAMIN PATCH & PRAYER WALL SUPPORT
When digestion is sensitive, swallowing supplements can add strain. PatchAid vitamin patches provide nutritional support without stressing the digestive tract, which can be helpful when managing symptoms.

Explore PatchAid here:
👉 http://www.patchaid.com/TEXASKK
Healing is not only physical. Prayer has been part of your journey from the beginning—calming your nervous system and strengthening your spirit.

Visit the Prayer Wall here:
👉 https://texaskkstompscancer.com/prayer-wall-esophagus-cancer/
WHEN TO PUSH FOR MEDICAL ANSWERS
Seek further evaluation if you experience:
- Worsening or constant pain
- Difficulty maintaining nutrition
- Nighttime symptoms
- Unintended weight loss
FINAL THOUGHTS: YOUR BODY IS NOT BROKEN
Your body carried you through cancer.
It adapted to survive.
It still communicates—sometimes loudly.
Duodenum spasm is not failure.
It is communication.
And you have learned how to listen—with patience, courage, and faith.